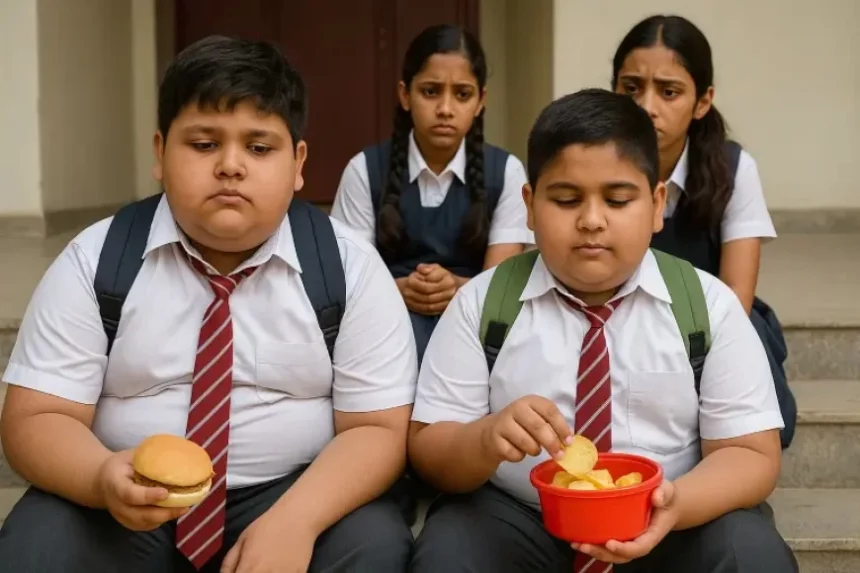India stands at a critical juncture in its fight for child health. Once known for under-nutrition, the nation now faces a paradox — while millions of children still suffer from malnutrition, a growing number are struggling with obesity. The UNICEF India Health Report 2025 has sounded a clear warning: obesity among school-aged children is rising at an alarming rate, potentially leading to a future public health crisis if not addressed urgently.
This issue is more than a health concern — it reflects deep changes in India’s lifestyle, food systems, education policies, and even national development priorities. Are India’s children eating themselves sick? Let’s explore the full picture — from history to modern challenges, from government efforts to parental responsibility, and what the future holds for the health of India’s next generation.
The Hidden Shift: From Undernutrition to Overnutrition
For decades, India was known as a country battling undernutrition. Government programs like the Integrated Child Development Services (ICDS), Mid-Day Meal Scheme, and Poshan Abhiyaan were launched to ensure children received enough nutrients to grow. However, while these programs continue, a silent nutritional transition has been underway.
According to UNICEF’s 2025 findings, nearly 14% of Indian school-aged children are now overweight or obese, compared to less than 4% two decades ago. The data paints a stark contrast — as India’s economy grows and urban lifestyles evolve, dietary habits are shifting from traditional, home-cooked meals to processed, calorie-dense fast foods.
The urbanization of diets, exposure to digital advertising, and limited physical activity have together created a generation consuming more calories than they burn. This transition, often described as the “nutrition trap,” is changing India’s health story.
Why Are Indian Children Becoming Obese?
The roots of childhood obesity in India lie in multiple interlinked factors — economic, social, cultural, and behavioral.
1. Urban Lifestyle and Sedentary Habits
Children today spend more time indoors — glued to screens, playing video games, or attending online classes. Physical play and outdoor activities have sharply declined, particularly in urban centers.
2. Processed and Packaged Foods
The rise of packaged snacks, sugary drinks, and fast-food chains has made high-calorie, low-nutrition food accessible to children of all income groups. Advertising targeted at children encourages consumption patterns that harm long-term health.
3. Parental Awareness Gap
Many parents still equate “chubbiness” with good health, not realizing that early obesity can lead to type-2 diabetes, heart disease, and joint issues even before adulthood.
4. School Canteen Culture
Despite government guidelines discouraging junk food sales in schools, many canteens still offer chips, samosas, and sugary beverages. UNICEF’s survey in 2025 found that over 60% of school canteens in metro cities sold unhealthy snacks daily.
5. Lack of Nutrition Education
Children rarely learn about healthy eating in schools. Nutrition remains an overlooked subject in India’s education system, even though it is a national priority under the National Education Policy (NEP) 2020 framework.
Historical Context: From Food Scarcity to Food Excess
In the 1950s–1980s, India’s major challenge was feeding its population. The Green Revolution solved hunger to a large extent, but it also shifted dietary patterns. With rising income and urban migration, refined carbohydrates, oils, and sugars became staples.
By the early 2000s, India’s middle class embraced modern consumerism — packaged snacks, fast-food chains, and sugary drinks became aspirational. Between 2010 and 2025, urban households’ processed food consumption increased by over 300%, according to NITI Aayog data.
Today, India faces a double burden of malnutrition — millions of children are still underweight in rural regions, while urban and semi-urban children face overnutrition and obesity.
What the UNICEF Obesity Report India 2025 Reveals
The latest UNICEF India Obesity Report 2025 highlights the growing imbalance in child nutrition. It calls obesity “the new face of malnutrition.” Key findings include:
- 14% of children aged 5–19 are overweight or obese.
- Urban boys are more likely to be obese than girls, but the gap is narrowing.
- Sedentary screen time among children has doubled since 2015.
- Rural obesity rates are rising faster than urban ones due to changing diets and access to processed foods.
- Only 1 in 5 parents can correctly identify signs of unhealthy weight gain in their children.
The report warns that if current trends continue, India could see a 70% rise in childhood obesity cases by 2035.
Real Stories: When Modern Diets Meet Indian Households
Take the story of Riya, a 12-year-old from Gurugram. Her parents, both working professionals, often rely on online food delivery. “Pizza or burgers have become weekend traditions,” her mother admits. Over time, Riya gained excess weight and began to feel fatigued. A doctor’s visit revealed she had early signs of insulin resistance.
In contrast, Aarav, a 10-year-old from a small town in Uttar Pradesh, used to eat homemade meals. But with a new mall and fast-food outlets opening nearby, his diet quickly changed. Aarav’s school friends often bring packaged chips and colas, making healthy tiffins look “boring.” Within a year, Aarav’s BMI crossed the normal range.
These stories highlight how globalization, technology, and lifestyle shifts are changing food culture across India — from metros to villages.
The Role of Schools and Educational Policies
Schools play a central role in shaping children’s habits. The Ministry of Education and FSSAI introduced guidelines in 2023 banning junk food in school canteens. However, enforcement remains patchy.
Several schools have taken innovative steps:
- Healthy Tiffin Initiatives: Some Delhi and Bengaluru schools encourage parents to follow weekly nutrition charts.
- Fitness Hours: Schools are including mandatory outdoor play or yoga sessions.
- Nutrition Clubs: A few CBSE institutions have introduced health awareness clubs to promote balanced eating.
The NEP 2020 also highlights the need for holistic health education, which includes mental and physical wellness. However, many educators say it will take years for such programs to reach every school.
Government Efforts and National Policies
The Indian government recognizes the challenge of obesity alongside malnutrition. Key initiatives include:
- Poshan 2.0 (2021–2026): Integrates nutritional interventions for women and children, focusing on balanced diets.
- Eat Right India Movement: Launched by FSSAI to promote safe, healthy, and sustainable food consumption.
- Fit India Movement: Encourages schools and workplaces to incorporate physical activity in daily routines.
- Ayushman Bharat – Health and Wellness Centres: Provide preventive healthcare services for children and adolescents.
- National Nutrition Mission: Aims to reduce both undernutrition and overnutrition by improving dietary diversity.
While these programs are impactful, experts argue that the implementation gap — especially in schools and households — remains the main barrier.
The Economic and Social Cost of Childhood Obesity
Childhood obesity is not just a health issue — it’s an economic one. A study by the Indian Council of Medical Research (ICMR) estimates that obesity-related diseases could cost India over ₹1.2 lakh crore annually by 2030 in lost productivity and healthcare expenses.
Socially, obese children face stigma and low self-esteem. Studies show that such experiences can lead to mental health issues like anxiety, depression, and eating disorders.
The crisis, therefore, affects education, employment, and even national productivity — making it a national development concern.
How Parents Can Take Action
Parents are the first line of defense against obesity. UNICEF recommends several actionable steps:
- Monitor eating patterns: Track not just quantity but quality of food.
- Limit screen time: Encourage outdoor activities or sports.
- Cook together: Teach children the value of fresh, home-cooked meals.
- Model healthy behavior: Children mimic adults — if parents eat healthy, they follow.
- Educate about marketing: Explain how ads manipulate food choices.
These small yet consistent actions can reshape a child’s relationship with food.
The Role of Media and Advertising
The influence of media on food habits is undeniable. Television, YouTube, and social media platforms bombard children with ads for sugary and processed foods.
In 2024, the Ministry of Information and Broadcasting introduced voluntary guidelines discouraging junk food advertising during children’s programming hours. However, without strict enforcement, many brands continue to target children indirectly through influencers and cartoon tie-ins.
A comprehensive policy regulating digital food advertising could be a game-changer in curbing obesity rates.
Looking Ahead: Can India Reverse the Trend?
Experts believe that India can still reverse this health trend — but only through collective action. Schools, parents, policymakers, and the food industry must work together.
Key Steps Forward:
- Nutrition Education in Curriculum – Make it mandatory in schools.
- Strict Junk Food Regulations – Enforce canteen and ad restrictions.
- Community Fitness Programs – Encourage public exercise spaces for children.
- Health Screening in Schools – Regular BMI checks for early intervention.
- Incentives for Healthy Food Brands – Promote Indian startups creating nutritious snacks.
If implemented effectively, these reforms can protect millions of children from lifelong health risks.
Building a Healthier Future for India’s Children
India’s journey from hunger to abundance is remarkable — but it comes with new responsibilities. The real success of national development will be measured not just in GDP, but in the health and happiness of its children.
Childhood obesity is reversible, but only if recognized as a national priority. It’s time for families, educators, and policymakers to act together, ensuring that India’s young generation grows not just smarter but healthier.
A future where every child has access to nutritious food, physical activity, and health education is possible — and it must begin today.